Many patients deciding to have cataract surgery wonder if cataracts grow back—and if so, how will they know? Doctors hear the question from patients all the time: “Are secondary cataracts possible?” In this article, we’ll review aspects of cataract formation, cataract surgery, ease patient fears of cataract recurrence, and educate you on the topic of secondary cataracts.
Before we can understand what a second cataract, or secondary cataract, is… we need to review what regular cataracts are, and how they are treated.
Overview of Cataract Anatomy and Treatment of Cataracts
A cataract is a clouding of the natural crystalline lens within the eye, most commonly associated with the aging process.1 Cataracts typically grow gradually over time, unless induced by trauma or other systemic/medical issues.
The crystalline lens is an oval-shaped, clear, avascular structure that helps to focus light rays on the retina. Anatomically, it is located posterior to the iris (the colored part of the eye) and anterior to the vitreous (the gel that causes ‘floaters’). Early in life, the lens is fairly pliable; it can change shape, which increases the focusing power of the eye (accommodation), thereby allowing near images to come into view. Over time, UV light absorption by the lens generates free radicals that cause molecular changes and alteration of lens proteins. This also increases accumulation of yellow pigments which may progress to a dark brown (“brunescence”) with time.1-3 As lens proteins break down and change, there is increased cloudiness (this cloudy lens is now a “cataract”).1-3
During cataract surgery, a very small, self-sealing incision is created in the eye and a specialized opening (capsulorhexis) is created in the lens capsule. An ultrasound probe is then used to break up and remove the cataract. Care is taken to preserve the lens capsule at the time of surgery so that it can hold the new artificial intraocular lens implant (IOL).1-3
What are Secondary Cataracts?
It is important to note that once removed, cataracts cannot grow back. Additionally, the IOL cannot develop cloudiness in the same way the natural crystalline lens can. What can happen, is that the lens capsule, (analogous in consistency to clear cellophane material), can become cloudy due to growth of residual microscopic lens cells inside of it—this is called “secondary cataract” and/or “posterior capsular opacification (PCO)”, and may occur in up to 50% or more of patients.1-7
Lens cells can spread across the posterior capsule behind the lens implant, resulting in cloudy vision that can be similar to the original cataract. However, it’s important to realize that it, in fact, is very different from the original cataract, and does not require a trip to the operating room for surgery to fix it.
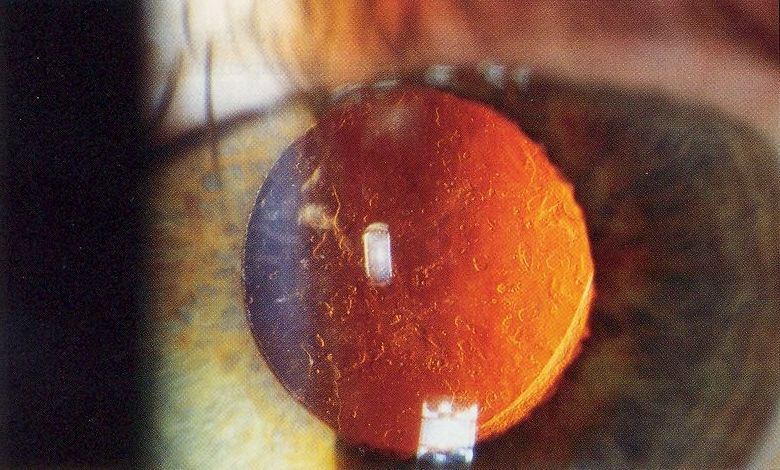
By Rakesh Ahuja, MD – Personal collection, CC BY-SA 2.5, Link
What are the symptoms of secondary cataracts?
Secondary cataracts are also known by the name “posterior capsular opacification”, or “PCO”. PCO can cause symptoms that are similar to cataracts. Some patients may complain of blurry vision; some may experience visual aberrations such as haloes, glare, and starbursts.6,7 These blurry vision symptoms can cause functional difficulties, such as driving at night, reading, or watching television.
There may be an increased incidence of PCO in patients who have a history of uveitis and diabetes. Blurry vision here is due to formation of multiple layers of lens epithelial cells (forming an opacity). In addition, PCO formation can also produce wrinkles in the posterior capsule, and associated distortion of vision.1,4,6,7
Does Insurance Cover Secondary Cataracts?
Yes. Medical insurance covers treatment for secondary cataracts. Virtually all commercial insurance plans and Medicare cover secondary cataracts and their treatment. Patients should expect to pay based on any co-pays or deductibles associated with their individual plan.
Secondary Cataract Treatment
Fortunately, PCO can be effectively treated to help restore clearer vision. This is done via use of a laser, called a neodymium-yttrium aluminum garnet (Nd:YAG) laser, in an outpatient setting.6-9 The pupil is dilated, and the laser is specifically focused on clearing the central area of PCO.6-9 Nd:YAG Laser is the most effective and painless procedure done for PCO; it does not touch the eye, no incisions are made, and no bleeding is involved. This laser treatment is different than femtosecond laser assisted cataract surgery.
Following laser treatment, the vision can be blurry for an hour or so; most patients can resume normal activities the same day, without restrictions. Although the procedure is relatively low risk, there are few case reports of damage to the retina, IOL, elevated intraocular pressure, and intraocular inflammation.6-9 However, adverse events are uncommon, and may be possibly related to the size of the laser opening that is created as well as total energy used.6-9 Patients have usually prescribed a mild anti-inflammatory eye drop to use for a few days post-treatment, and followed up within a few weeks.
So while there are different types of cataracts and a secondary cataract can cause similar symptoms to a patient’s original cataracts, it is a very different, and much easier to fix, condition.
References
- Cataracts. National Eye Institute. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/cataracts. 2019
- Remington, Lee Ann, editor. “The Crystalline Lens.” Clinical Anatomy of the Visual System, Elsevier Health Sciences, 2014, pp. 92–101.
- The physical basis for transparency of the crystalline lens, Invest Ophthalmol 1:493, 1962
- Types of Cataract. National Eye Institute. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/cataracts/types-cataract. 2019
- Yanoff, Myron, and Joseph W. Sassani, editors. “Surgical and Nonsurgical Trauma.” Ocular Pathology, 6th ed., Mosby, 2009, pp. 129–130.
- Hayashi K, Hayashi H, Nakao F, et al. Posterior capsule opacification after cataract surgery in patients with diabetes mellitus. Am J Ophthalmol. 2002; 134:10.
- Awasthi N, Guo S, Wagner J. Posterior Capsular Opacification: A Problem Reduced but Not Yet Eradicated. Arch Ophthalmol. 2009;127(4):555-562
- TM, Devlin HD, Hillon B. Use of Nd:YAG laser capsulotomy. Surv Ophthalmol. 2003;48(6): 594-612
- Karahan E, Er D, Kaynak S. An Overview of Nd:YAG Laser Capsulotomy. Med Hypothesis Discov Innov Ophthalmol. 2014;3(2)